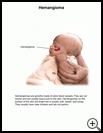
Hemangioma
________________________________________________________________________
KEY POINTS
- Hemangiomas are growths made of extra blood vessels. They are not cancer. They are usually just on the skin but can be found on other body parts also.
- Most hemangiomas get smaller and eventually go away without treatment. Your child may need medicine, laser treatments, or surgery.
- Follow the instructions your child's healthcare provider gives you. Make sure you know when your child should come back for a checkup.
________________________________________________________________________
What is a hemangioma?
Hemangiomas are growths made of extra blood vessels. They are not cancer and are usually found just on the skin, although some may be found in the eye, mouth, liver, digestive tract, or other parts of the body. Most hemangiomas appear at birth or within a week or 2 after birth. They often get bigger during the first 6 months of life and may go away on their own by age 3 to 5 years. Usually a child has just 1 hemangioma.
What is the cause?
The exact cause of hemangiomas is not known. They tend to run in families and happen more often in lighter skinned babies than darker skinned babies. Hemangiomas are more common in girls than boys and are more common in babies who are born early.
What are the symptoms?
Hemangiomas on the surface of the skin are bright red or purple, soft, raised, and lumpy. They usually have clear borders. A hemangioma can be as small as a pinhead or grow to 7 inches (20 cm) across. They are usually not painful. They are most often on the head, chest, or upper back.
Some hemangiomas are deeper in the skin. They often look bluish, and the borders are less clear. Most of these hemangiomas are on the head or neck.
A hemangioma may start as a small red bump but then quickly start getting bigger. Between 12 and 18 months of age, the hemangioma may start turning gray. This is a sign that it is starting to go away.
Hemangiomas inside the body may not cause any symptoms. They are usually found during a test looking for another problem. Some medicines, such as synthetic hormones, may make these hemangiomas grow. If they do cause symptoms, they may include:
- Pain in the belly, particularly on the upper right side
- A lump in the area of the hemangioma
Hemangiomas inside the body may cause breathing problems, heart failure, or other problems, depending on the size and location of the hemangioma.
How is it diagnosed?
Your healthcare provider will ask about your child's symptoms and medical history and examine your child. Most hemangiomas can be diagnosed by your child’s healthcare provider without any tests.
If your child has a very large hemangioma that is causing pain or interfering with normal activities, has more than 2 or 3 hemangiomas on the skin, or has a deep hemangioma, your child may have other tests to confirm the diagnosis and to check for other hemangiomas inside the body. Tests may include:
- An ultrasound, which uses sound waves to show pictures of the area under the hemangioma
- MRI, which uses a strong magnetic field and radio waves to show detailed pictures of the internal organs
- Biopsy, which is the removal of a small sample of tissue for testing
How is it treated?
Most hemangiomas get smaller and eventually go away without treatment. Your child may need medicine or laser treatments to shrink the hemangioma or surgery to remove it if:
- It is large enough to cause problems. For example, it may block the mouth, nose, eye, or ear and cause problems with feeding, breathing, vision, or hearing.
- It causes bleeding or pain, or seriously affects the way your child looks
- It causes other problems such as heart failure
Your child’s healthcare provider may refer your child to a specialist for treatment.
How can I take care of my child?
Follow the instructions your child’s healthcare provider gives you. Ask your provider:
- How long it will take to recover
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup.
It may be upsetting to you if your child's hemangioma seriously affects the way your child looks. It may be hard for you when strangers stare or ask questions. Talk to your child’s healthcare provider about what to expect. Many families find that counseling can help the parents and the child, particularly before your child starts school.
Last modified: 2020-11-25
Last reviewed: 2018-03-01