Sickle Cell Anemia
________________________________________________________________________
KEY POINTS
- Sickle cell anemia is an inherited life-long condition caused by abnormal, sickle-shaped red blood cells. The abnormal blood cells are stiff and sticky. They can block blood flow in the blood vessels of the limbs and organs. Blocked blood flow can cause pain and organ damage and can raise the risk for infection.
- Treatment includes medicines, blood transfusions, and sometimes bone marrow transplants.
- To try to prevent sickle cell crises, it helps to help your child avoid strenuous exercise, smoking and using e-cigarettes, and dehydration from excessive sweating, vomiting, or diarrhea.
_________________________________________________________________
What is sickle cell anemia?
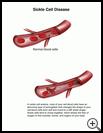
Sickle cell anemia is a blood disease that causes abnormal red blood cells. Sickle cell anemia is an inherited, lifelong disease. Red blood cells contain an iron-rich protein called hemoglobin. This protein carries oxygen from your lungs to the rest of your body. If your child has sickle cell anemia, most of the red blood cells have an abnormal type of hemoglobin called hemoglobin S. Hemoglobin S changes the shape of your red blood cells. Instead of being soft and round, the cells are a stiff crescent (sickle) shape. This shape makes it harder for the blood cells to pass through small blood vessels. Sickle cells are stiff and sticky. They can block blood flow in the blood vessels of the limbs and organs causing pain and organ damage. This can raise the risk for infection.
Normal blood cells usually last about 4 months and are always being replaced. Normal red blood cells look like doughnuts without holes in the center. They move easily through your blood vessels. The abnormal blood cells are fragile and last only a few weeks. Your child’s body may not be able to make new red blood cells fast enough. This can cause a shortage of red blood cells. The shortage of red blood cells is called anemia.
What is the cause?
Sickle cell anemia is inherited. Genes are in each cell of the body. They contain the information that tells the body how to develop and work. Changes in the genes can be passed from parents to children. If your child inherited the gene from both parents, it is likely your child will have the disease. If your child inherited the faulty gene from just 1 parent, usually your child will not have the disease, but can pass the gene on to any of his or her children (sickle cell trait).
People from Africa, South or Central America, Caribbean islands, Turkey, Greece, Italy, India, and Saudi Arabia have a high risk of the disease. In the US, sickle cell anemia affects mainly African Americans and Hispanics/Latinos.
What are the symptoms?
Babies are born with a kind of hemoglobin that protects the red blood cells from sickling right away. Around age 4 to 5 months, this newborn hemoglobin is replaced by "adult" hemoglobin and the cells start to sickle. After 4 months of age, symptoms are often brought on by an infection.
The symptoms are different from person to person and can range from mild to severe. Most people with sickle cell anemia have times when they have symptoms and times when they do not have symptoms. The most common symptoms are related to anemia and pain.
Symptoms of anemia may include:
- Feeling tired all the time
- Shortness of breath, dizziness, headaches, coldness in hands or feet
- Skin more pale than usual
- Yellowing of skin or eyes
When abnormal red blood cells block the flow of blood and cause symptoms, it is called a “crisis.” The most common symptom of a sickle cell crisis is pain. The pain is usually felt in the part of the body where the sickling cells are blocking blood flow. Crises may start suddenly and last from a few days to several weeks. The pain may be mild to severe. Although not as common as a crisis, you may also have ongoing pain, which is often felt in the bones.
Toddlers and children may have frequent pain with or without any other signs of illness.
Sickle cells crises can cause damage to many organs. Damage to the spleen can make it easier to get an infection and harder to fight certain infections. Symptoms may include:
- Ongoing fever higher than 101°F (38.3°C)
- Cough that produces mucus
- Vomiting
- Diarrhea
- Stomach pain
What are the complications of sickle cell anemia?
Abnormal red blood cells can cause problems in any part of your child’s body. Some of the possible problems are:
- Infections such as pneumonia or meningitis
- High blood pressure in the lungs that can cause trouble breathing and heart damage
- Acute chest syndrome, which is a life-threatening lung problem that causes fever, chest pain or pressure, cough, or shortness of breath
- Heart attack
- Kidney or bone infections
- Gallstones
- Loss of vision caused by damage to blood vessels in the eyes
- Hip and shoulder joint damage
- Stroke
- Damage to tissues in the penis
- Too much blood collecting in the spleen
- Painful leg sores
- Blood clots
How is it diagnosed?
In the US, sickle cell anemia is usually diagnosed at birth with a newborn screening test.
If your child has never been screened for sickle cell anemia, your child may have blood tests to look for anemia, sickle-shaped red blood cells, and abnormal hemoglobin.
How is it treated?
Sickle cell anemia has no common cure. Treatments may improve the anemia and lower complications. A bone marrow or stem cell transplant may offer a cure for a small number of people.
If your child has sickle cell anemia, it is important for you to work with healthcare providers who have experience treating sickle cell disease in children.
Treatments may include:
- Pain medicine
- Medicine to try to prevent sickle cell crisis. Taken daily, this medicine may help your child have fewer crises. It can also shorten how long each crisis lasts.
- Vaccines such as Haemophilus influenzae type b, hepatitis A and B, influenza (flu), COVID-19, meningitis, and (pneumococcal) pneumonia shots to prevent infection. People with sickle cell anemia are more likely to have serious infections, ranging from flu to pneumonia. Infections can cause a sickle cell crisis.
- Blood transfusions
- Antibiotic medicine
- Folic acid to help make red blood cells
- Bone marrow transplant
- Gene therapy is being studied as a possible treatment for sickle cell anemia. Gene therapy adds a healthy version of a hemoglobin gene to blood stem cells.
- Medicine to remove extra iron in your child’s body. Your child should not take iron supplements. Sickle cell anemia is not caused by too little iron in the blood. Taking iron supplements can be harmful because the extra iron builds up in your child’s body and can damage the organs.
How can I take care of my child?
To try to prevent sickle cell crises, your child should avoid things that lower the blood oxygen such as:
- Strenuous exercise
- Extreme hot or cold temperatures
- High altitude
- Tight clothing
- Things that can make the blood vessels narrower such as:
- Some medicines
- Cigarette smoking
- Illegal drugs such as cocaine
Also, try to avoid dehydration. A loss of too much fluid from your child's body can cause sickling. Your child may lose too much fluid from:
- Heavy sweating
- Urinating a lot, which can happen with uncontrolled diabetes or taking diuretics (water pills)
- Fever
- Vomiting or diarrhea
- Help your child stay physically active as advised by your child’s provider. Your child should rest when tired.
- Talk to your child about the risks of smoking, using e-cigarettes, drinking alcohol, and using drugs. Smoking can worsen poor blood circulation.
- Stay up to date with the recommended immunizations (shots) for your child including flu and COVID-19. Ask your healthcare provider about any other vaccines your child or your family may need.
Encourage your child and family to talk about how you all feel with your health care team. Talking to a professional counselor also can help. Teen support groups and family and individual counseling are ways to support teens who have sickle cell anemia.
Follow the full course of treatment prescribed by your child’s healthcare provider. Ask your provider:
- How and when you will get your child’s test results
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
If your child has sickle cell anemia, learn as much about the disease as possible. This will help you recognize early signs of problems, such as fever or chest pain, and seek early treatment. Sickle cell centers and clinics can give you facts and counseling to help you handle the stress of coping with your child's disease.
Make sure you know when your child should come back for a checkup.
How can I help prevent sickle cell anemia?
People who have the gene may pass the disease on to their children. Couples can get tested for the gene that causes sickle cell disease. If one of you has the gene, you will need to decide whether to take the chance of passing the disease on to your children. You may want to talk with a genetic counselor if anyone in your family has sickle cell anemia.
For more information, contact:
- National Organization for Rare Disorders: Sickle Cell Disease
203-744-0100
https://rarediseases.org/rare-diseases/sickle-cell-disease
Last modified: 2022-01-03
Last reviewed: 2019-03-07