Staph Infection
________________________________________________________________________
KEY POINTS
- Staphylococcus, or staph, is a kind of bacteria that can cause skin, bone, muscle, or joints infections, and rarely, other serious infections such as pneumonia and heart infections.
- Your child may need to take antibiotic medicine by mouth, or your child may need to be in the hospital with IV antibiotic medicine. Tell your healthcare provider if people living with your child have been diagnosed with methicillin-resistant staphylococcus, or MRSA.
- Ask your child’s healthcare provider what symptoms or problems you should watch for and what to do if your child has them.
________________________________________________________________________
What is a staph infection?
Staphylococcus, or staph, is a kind of bacteria. Staph can cause skin infections such as impetigo, boils, and cellulitis. The bacteria can also infect bone, muscle, or joints. Rarely, staph may cause other serious infections such as pneumonia and heart infections.
What is the cause?
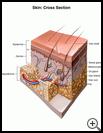
Staph bacteria usually live on the skin without hurting your child. However, if the bacteria get into the deeper layers of the skin, they may cause an infection. This can happen if your child has a skin condition like eczema, or if your child has a scratch, scrape, insect bite, or other irritation that causes a break in the skin.
What are the symptoms?
For common skin infections, such as impetigo or boils, symptoms may include:
- Small areas of swelling and redness such as pimples or blisters
- Pain or tenderness
- Pus coming from the infected area
- Yellowish crusting of the area
Deeper skin infection (cellulitis) can result in:
- A larger area of swelling, pain, warmth, and redness that may spread quickly
- Fever
How is it diagnosed?
Your healthcare provider will ask about your child’s symptoms and medical history and examine your child. Tests may include:
- Tests of a sample of pus
- A biopsy, which is the removal of a small sample of infected tissue for testing
- Blood tests
How is it treated?
For many skin infections, draining the pus from the area is all that is needed. Mild infections on the surface of the skin may be treated with a medicine put on the skin. For infections such as impetigo and cellulitis, your child may need to take an antibiotic medicine by mouth for 1 to 2 weeks. More serious infections may need to be treated in the hospital with IV antibiotic medicine.
The widespread use of antibiotic medicine has caused some of these bacteria to change and become resistant to antibiotic medicines. Resistance means that the bacteria cannot be killed by these antibiotic medicines. Methicillin-resistant staphylococcus, or MRSA, is a type of staph that is very hard to treat with most antibiotic medicines. Be sure to tell your healthcare provider if people living with your child have been diagnosed with MRSA.
How can I take care of my child?
Follow your healthcare provider’s instructions. Give medicine exactly as prescribed. If your child stops taking the medicine too soon, the infection may come back. If your child has side effects from the medicine, talk to your child’s provider. In addition:
- Ask your child’s healthcare provider how to care for the infected area. For example, your provider may recommend keeping the infected area up on pillows (above the level of the heart) when your child sits or lies down to decrease swelling and pain.
- Put a warm, moist towel on the reddened area a few times a day for a day or two.
- Give your child pain medicine, such as ibuprofen, as directed by your provider. Nonsteroidal anti-inflammatory medicines (NSAIDs), such as ibuprofen, may cause stomach bleeding and other problems. Read the label and give as directed. Check with your healthcare provider before you give any medicine that contains aspirin or salicylates to a child or teen. This includes medicines like baby aspirin, some cold medicines, and Pepto-Bismol. Children and teens who take aspirin are at risk for a serious illness called Reye syndrome.
Ask your child’s provider:
- How and when you will get your child’s test results
- How long it will take your child to recover
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup.
How can I help prevent staph infections?
To help prevent skin infections, teach your child to do the following:
- Keep hands clean by washing well with soap and water or using an alcohol-based hand sanitizer.
- Clean cuts, scrapes, and other skin injuries well with soap and water.
- Keep wounds and sores clean and dry. You may need to cover some wounds with a bandage to keep them clean and dry. Change the bandage daily and more often if it gets dirty or wet.
- Avoid contact with other people's wounds or bandages.
- Don’t share personal items such as towels or razors.
- Take care of your child’s health. Make sure your child eats a variety of healthy foods and gets enough sleep and physical activity every day. Talk to your child about the risks of smoking, using e-cigarettes, drinking alcohol, and using drugs.
- If your child has diabetes, follow your provider’s instructions for good skin care and keep your child’s blood glucose (sugar) under good control.
- See your healthcare provider for treatment as soon as possible if a wound or sore shows signs of infection. Signs of infection include new or worse redness, swelling, pain, warmth, or drainage from the wound.
Last modified: 2022-01-03
Last reviewed: 2019-10-07