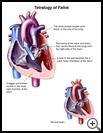
Tetralogy of Fallot
________________________________________________________________________
KEY POINTS
- Tetralogy of Fallot is group of 4 birth defects in the heart. These 4 problems mean that not enough blood can get to the lungs to get oxygen. The oxygen-poor blood is pumped to the rest of the body.
- This birth defect is usually treated with surgery in childhood.
- Treatment may include medicines and regular follow-up visits. If your child has a damaged heart valve that is causing severe symptoms, your child may need valve replacement surgery.
- Stay up to date with the recommended immunizations (shots) for your child including flu and COVID-19. Ask your healthcare provider about any other vaccines your child or your family may need.
________________________________________________________________________
What is Tetralogy of Fallot?
Tetralogy of Fallot (ToF) is group of birth defects in the heart. The heart has 4 sections, or chambers. There are 2 upper chambers each called atria, and the 2 lower chambers are called ventricles. The heart muscle squeezes to push blood through these 4 chambers to the lungs and the rest of the body. Blood flows from the right atrium into the right ventricle, and the right ventricle pumps it to the lungs. As it passes through the lungs, the blood picks up oxygen and leaves behind carbon dioxide. Then the blood flows back to the heart and into the left atrium, and from there into the left ventricle. The left ventricle pumps the blood out to the rest of the body, with a small amount going to the heart muscle itself. The heart pushes blood out through the arteries and blood returns to the heart through the veins.
The heart has 4 valves that open and close with each heartbeat to keep the blood flowing in the right direction through the heart. They are made of thin tissues that open and close easily. The valves are closed while the chambers fill with blood, and then they open to push blood out.
ToF means that the heart has these 4 problems:
- A bigger and thicker muscle in the lower right chamber of the heart
- A hole in the wall between the 2 lower heart chambers of the heart
- An aorta in the wrong part of the heart. The aorta is the large artery that carries blood from the heart to the rest of the body.
- Narrowing of the valve and artery that carries blood to the lungs from the right side of the heart
These 4 problems mean that not enough blood can get to the lungs to get oxygen. The oxygen-poor blood is pumped to the rest of the body.
What is the cause?
The cause of this birth defect is not known. It is more common in babies with Down syndrome.
What are the symptoms?
Children with this birth defect often have a blue color of their skin, lips, and fingernails. The blueness may appear at birth or soon after. Babies may have spells during which they turn blue, breathe very fast, and cry. They may pass out.
Older children often get short of breath during activities and may tire easily. They may squat during an activity to help them catch their breath. These symptoms happen because the children are not getting enough oxygen. Not enough blood is flowing to the lungs to pick up the oxygen their body needs.
How is it diagnosed?
Your healthcare provider will ask about your child's symptoms and medical history and examine your child. Children with this defect usually have a heart murmur, which your healthcare provider can hear with a stethoscope. A heart murmur is a whooshing sound as blood moves through the heart.
Tests may include:
- An echocardiogram, which uses sound waves (ultrasound) to see how well the heart is pumping
- Heart catheterization, which uses a small tube called a catheter inserted into a blood vessel, contrast dye, and X-rays to look at the blood vessels and heart
How is it treated?
The problem is treated with surgery. If your baby is too sick or there are other problems, a surgeon can place a small tube, called a shunt, that lets more blood enter the lungs and pick up oxygen. Then more surgery can be done at a later time to correct the defect.
After surgery, most children have few limits on their activities. Some may need to take medicine to control their heart rate and to help their heart pump better. Later in life, they may have other heart problems.
How can I take care of my child?
Your child may need to have regular follow-up visits with a specialist in congenital heart disease. Follow your child’s healthcare provider's instructions. Stay up to date with the recommended immunizations (shots) for your child including flu and COVID-19. Ask your healthcare provider about any other vaccines your child or your family may need.
Ask your child’s provider:
- How and when you will get your child’s test results
- How long it will take for your child to recover
- How to take care of your child at home
- If your child should take antibiotic medicine to prevent infection before having dental work or procedures that involve the rectum, bladder, or vagina
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
Last modified: 2022-01-03
Last reviewed: 2019-03-25