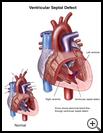
Ventricular Septal Defect
________________________________________________________________________
KEY POINTS
- A ventricular septal defect (VSD) is a hole between the lower 2 chambers of the heart. This makes the heart and lungs work harder.
- Your child’s healthcare provider will advise treatment based on the symptoms and size of the defect. Medium and large ventricular septal defects may need to be fixed with surgery or heart catheterization.
- Follow your child’s healthcare provider's instructions. Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
_______________________________________________________________________
What is a ventricular septal defect?
A ventricular septal defect (VSD) is a hole between the lower 2 chambers of the heart.
The heart has 4 sections, or chambers. The upper chambers are called atria, and the lower chambers are called ventricles. The wall between the 2 ventricles is called the ventricular septum.
Normally, blood flows from the right atrium into the right ventricle, and the right ventricle pumps it to the lungs. When there is a hole in the ventricular septum, oxygen-rich blood from the left ventricle flows into the right ventricle. Then it is pumped back to the lungs, even though this blood does not need oxygen. This makes the heart and lungs work harder.
What is the cause?
A VSD is found most often in babies. It happens before birth and is the most common birth defect of the heart. Often it is the only defect, but sometimes there are other heart defects as well. Most of the time the cause of the birth defect is not known. Heart defects may be inherited, which means that they are passed from parents to children through their genes. Genes are inside each cell of your body. They contain the information that tells your body how to develop and work.
Rarely, an injury to the heart or a heart attack may cause a VSD.
What are the symptoms?
If the defect is mild, there may be no symptoms. It may be found only when being tested for something else. Healthcare providers can hear the murmur with a stethoscope. Many defects cause a whooshing sound, called a murmur, as blood moves through the heart.
Large defects may cause symptoms. Even if the defect is large, a child often does not have symptoms until several weeks after birth. Symptoms may include:
- Not feeding well and not growing normally
- Sweating
- Faster breathing rate or trouble breathing
- Fever or coughing up mucus
- Being sleepy all the time
How is it diagnosed?
Your healthcare provider will ask about your child’s symptoms and medical history and examine your child.
Tests may include:
- A chest X-ray
- An ECG (also called an EKG or electrocardiogram), which measures and records the heartbeat
- An echocardiogram, which uses sound waves (ultrasound) to see how well the heart is pumping
Your child may have other tests to check for possible causes of the symptoms.
How is it treated?
Your healthcare provider will advise treatment based on the symptoms and size of the defect.
A small defect may never cause any symptoms or problems. The smaller the defect, the greater the chance that it will close on its own, usually in the first years of a child’s life. People with a small VSD may lead normal lives.
Medium and large ventricular septal defects may need to be fixed with surgery or heart catheterization.
Two types of surgery may be done to close the defect:
- Heart catheterization, which uses a small tube called a catheter inserted into a blood vessel, contrast dye, and X-rays to look at the blood vessels and heart. The healthcare provider will use tools put through the catheter to repair the defect. The hole may be closed by sewing it, patching it with a small piece of tissue from another part of the heart, or by plugging the hole with a small metal or plastic device.
- Open heart surgery to close the defect may be needed if it is large or if there are other heart defects.
If your child has symptoms, medicines will be given to help the heart pump better until your child has surgery.
How can I take care of my child?
Follow your child’s healthcare provider's instructions. Ask your provider:
- How and when you will get your child’s test results
- How long it will take for your child to recover
- If there are activities your child should avoid
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
Last modified: 2018-11-01
Last reviewed: 2018-10-29