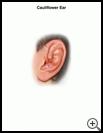
Cauliflower Ear: Teen Version
________________________________________________________________________
KEY POINTS
- Cauliflower ear is a lumpy or puffy outer ear that does not go away. It is caused by injury.
- Treatment may include draining blood from the ear, bandaging to prevent swelling, or plastic surgery.
________________________________________________________________________
What is cauliflower ear?
Cauliflower ear is a lumpy or puffy outer ear that does not go away. It is also called wrestler’s ear or boxer’s ear.
What is the cause?
Cauliflower ear is caused by injury. It may be caused by repeatedly being hit in the ear in sports such as boxing and rugby. It may also be caused by ongoing rubbing or pressure on the ear in sports such as wrestling. It may also be caused by child abuse.
The injuries can cause blood to collect between the skin and cartilage in the ear. Cartilage is the tough but flexible tissue that gives your ear its shape. The skin can pull away from the cartilage. If your ear is injured many times, scar tissue forms and can change the way your ear looks. The scar tissue can block blood supply and make the ear bumpy and pale and look like a cauliflower.
What are the symptoms?
Symptoms may include pain, bruising, and swelling on and around the ear. Rarely there may be hearing loss.
How is it diagnosed?
Your healthcare provider will ask about your symptoms and medical history and examine you.
How is it treated?
If blood has collected between the skin and cartilage in your ear, it may need to be drained by your healthcare provider as soon as possible. Quick treatment may prevent lasting damage to the tissue. Your provider will put a tight dressing on your ear to help decrease swelling and keep fluid from building up again. Your healthcare provider may prescribe antibiotic medicine to prevent infection.
If scar tissue has already formed, you will need plastic surgery on the ear to make it look normal.
How can I help prevent cauliflower ear?
Use protective head gear for sports such as wrestling or boxing. If your ear is injured, get prompt treatment to prevent cauliflower ear.
Last modified: 2019-10-29
Last reviewed: 2018-12-18