Skin Biopsy
________________________________________________________________________
KEY POINTS
- A skin biopsy is a procedure to remove a small piece of skin to test and diagnose a skin problem.
- Ask your child’s provider how long it will take to recover and how to take care of your child at home.
- Make sure you know what symptoms or problems you should watch for and what to do if your child has them.
________________________________________________________________________
What is a skin biopsy?
A skin biopsy is the removal of a small piece of skin for testing. After the skin is removed, it is sent to a lab where it is examined under a microscope or tested.
When is it used?
A skin biopsy may be done to diagnose or help treat skin problems such as:
- Psoriasis, which is rough, dry, thick patches of skin that may be covered with silvery-white scales
- Scleroderma, which is a disease that causes the skin to get thick, hard, and sometimes numb
- Blisters
- Skin cancer
- Skin infection
- Skin tags, moles, rashes with no clear cause, or other growths on your child’s skin
- Stevens-Johnson syndrome, which causes skin sores
- Warts
How do I prepare my child for this procedure?
- Your child may or may not need to take regular medicines the day of the procedure. Tell the healthcare provider about all medicines and supplements your child takes. Some products may increase the risk of side effects. Ask the healthcare provider if your child needs to avoid taking any medicine or supplements before the procedure.
- Tell the healthcare provider if your child has any food, medicine, or other allergies such as latex.
- Follow any other instructions your child’s provider gives you.
- Ask any questions you have before the procedure. You should understand what your child’s provider is going to do. You have the right to make decisions about your child’s healthcare and to give permission for any tests or procedures.
What happens during the procedure?
This procedure may be done at your child’s healthcare provider’s office or a surgery center.
Your child’s provider may numb your child’s skin with a spray or shot of local anesthetic to keep your child from feeling pain during the biopsy.
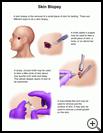
There are different ways to do a skin biopsy.
- A knife called a scalpel may be used to take a small piece of skin, a lump, or a sample from an abnormal area.
- A sharp, circular knife may be used to take a little circle of skin about one quarter inch wide and deep. This allows deeper layers of skin to be examined. This is called a punch biopsy.
- A razor-blade-like tool may be used to remove just the surface of skin. It may also be used to remove a small growth on the skin. This is called a shave biopsy.
What happens after the procedure?
Your child may have some soreness around the biopsy area for 1 or 2 weeks. Your child may have a small scar from the biopsy.
Follow your child’s provider's instructions for taking care of your child’s wound. Ask your child’s healthcare provider:
- How and when you will get your child’s test results
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
What are the risks of this procedure?
Every procedure or treatment has risks. Some possible risks of this procedure include:
- Your child may have problems with anesthesia.
- Your child may have infection or bleeding.
Ask your child’s healthcare provider how these risks apply to your child. Be sure to discuss any other questions or concerns that you may have.
Last modified: 2021-12-07
Last reviewed: 2017-12-21