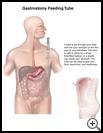
Gastrostomy Feeding Tube Placement
________________________________________________________________________
KEY POINTS
- Gastrostomy feeding tube placement is a procedure for putting a tube directly into your child’s stomach through the belly wall to give your child fluids, liquid food, and medicines.
- Ask your provider how long it will take to recover and how to take care of your child at home.
- Make sure you know what symptoms or problems you should watch for and what to do if your child has them.
________________________________________________________________________
What is gastrostomy feeding tube placement?
Gastrostomy feeding tube placement is a procedure for putting a tube directly into your child’s stomach through the belly wall. The tube can be used to give your child fluids, liquid food, and medicines.
When is it used?
This procedure may be done if your child cannot eat or swallow normally. For example, your child may need a gastrostomy feeding tube if:
- Your child cannot swallow or cannot burp on his own.
- Your child is unable to eat enough food to gain weight and grow.
- Your child cannot eat enough food, or your child’s body is not getting all the vitamins, minerals, and other nutrients it needs. For example, your child may be getting medical treatment, such as chemotherapy or radiation therapy, that is making it hard for your child to eat enough.
Before having a gastrostomy feeding tube, your child may have a temporary feeding tube that is passed through the nose or mouth and down into the stomach. A gastrostomy tube is more comfortable than a nose tube and it may be used if your child needs a feeding tube for a longer time.
Ask your healthcare provider about your child’s choices for treatment and the risks.
How do I prepare my child for this procedure?
- Tell your provider if your child has any food, medicine, or other allergies such as latex.
- Your child may or may not need to take regular medicines the day of the procedure. Tell the healthcare provider about all medicines and supplements your child takes. Some products may increase your child’s risk of side effects. Ask the healthcare provider if your child needs to avoid taking any medicine or supplements before the procedure.
- Your provider will tell you when your child should stop eating and drinking before the procedure, including fluid and foods that are given through a temporary feeding tube. This helps to keep your child from vomiting during the procedure.
- Follow any instructions your child’s healthcare provider may give you.
- Ask any questions you have before the procedure. You should understand what the healthcare provider is going to do. You have the right to make decisions about your child’s healthcare and to give permission for any tests or procedures.
What happens during the procedure?
Your child will be given a local, regional, or general anesthetic before the procedure to keep from feeling pain. Local and regional anesthesia numb part of the body while your child stays awake. Your child may be given medicine with the local or regional anesthetic to help relax. General anesthesia relaxes the muscles and puts your child into a deep sleep.
An endoscope is a slim, flexible, lighted tube passed through your child’s mouth to look at the esophagus and stomach. Your child’s healthcare provider will use the endoscope during the procedure to see the inside of your child’s stomach.
The healthcare provider will make a small cut over the stomach usually on the left side of your child’s belly and put a tube in the stomach. The tube will be held in place by a small fluid-filled balloon or a plastic cap inside your child’s stomach. The healthcare provider will attach the tube inside the stomach and to your child’s skin. The endoscope is removed at the end of the procedure. A small bandage will be placed around the tube and over the skin.
What happens after the procedure?
This procedure may be done at a surgery center or hospital. Your child may go home the same day, or may stay in the hospital for several days, depending on your child’s condition. You will be taught how to use and care for the feeding tube before your child leaves the hospital. It can usually be used within 12 to 24 hours after the procedure. Your child may have some soreness where the tube goes into the belly.
Liquid food may be passed through the tube into your child’s stomach with a special syringe or with a pump. You will be given instructions for how much, when, how long, and how often you should give liquid food and other fluids. If your child needs the tube for a long time, it may need to be replaced with a new tube some time later. Replacing the tube is a procedure that often can be done in a healthcare provider's office.
Discuss your child’s medicines with your child’s healthcare provider. You can get many medicines in liquid form instead of pills and they can be given through the feeding tube with a syringe. Other medicines can be dissolved in water and given through the feeding tube. Always flush the feeding tube with water after putting medicines or food in it to keep the tube from getting clogged.
Your child may have changes in bowel movements. Your child’s bowel movements may be looser, or they may be less frequent and harder than normal.
Make sure that your child’s feeding tube is carefully secured to the belly. A feeding tube should not keep your child from returning to school or most activities. If you have questions about this, ask your child’s healthcare provider.
Follow the healthcare provider's instructions. Ask your child’s provider:
- How long it will take to recover
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
What are the risks of this procedure?
Every procedure or treatment has risks. Some possible risks of this procedure include:
- Your child may have problems with anesthesia.
- Your child may have an infection or bleeding.
- Other parts of your child’s body may be injured during the procedure.
Ask your healthcare provider how these risks apply to your child. Be sure to discuss any other questions or concerns that you may have.
For more information, contact:
- United Ostomy Associations of America
800-826-0826
https://www.ostomy.org/
Last modified: 2021-12-07
Last reviewed: 2021-06-17