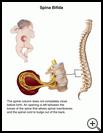
Spina Bifida
________________________________________________________________________
KEY POINTS
- Spina bifida is a birth defect that happens when the spinal column does not completely close before birth.
- Spina bifida can cause mild to severe symptoms.
- Depending on how severe the symptoms, treatment can include surgery, braces, walkers, medicine, or other therapies.
________________________________________________________________________
What is spina bifida?
Spina bifida is a birth defect that happens when the spinal column does not completely close before birth. An opening is left between the bones of the spine (vertebrae) that allows spinal membranes and sometimes the spinal cord to bulge out of the back. This can damage nerves and the spinal cord and cause problems.
Spina bifida can be mild to severe. It’s most severe when the spinal cord sticks out and is not covered by skin. Children with the more severe form of spina bifida may have:
- A loss of full use of their legs (paralysis)
- Problems with learning
- Trouble controlling their bowel and bladder
- Kidney problems
- A buildup of fluid around the brain
What is the cause?
The exact cause of spina bifida is not known. The defect usually happens in the first month of pregnancy. Many things may cause it such as a genetic problem that the child has at birth, medicines the mother has taken, the environment, and the mother’s diet. The risk of spina bifida is higher if a mother doesn’t get enough of the vitamin called folic acid during pregnancy.
Women who have one child with spina bifida have a greater chance of having another child with the same problem.
What are the symptoms?
Symptoms caused by spina bifida depend on how severely the spinal cord and nerves are damaged. For example, your child may have:
- A loss of feeling in part of the body
- Weakness of the hips, feet, or legs
- Partial or complete loss of use of the legs (paralysis)
- Bladder problems
Your child may have a tuft or clump of hair or a small dimple or birthmark on the skin over the part of the spine with the defect. Or there may be a fluid-filled sac on the baby’s back.
How is it diagnosed?
Tests may be done during pregnancy to check for spina bifida. A blood test called a quad screen, done during the second trimester, includes a measurement of the level of a substance called alpha fetoprotein (AFP). The levels of AFP may be especially high if a baby has spina bifida.
After birth your child’s healthcare provider will examine your child. Tests may include different kinds of scans and nerve tests.
How is it treated?
Treatment includes surgery to close the open area of the spine and watching the child's growth and development. If only the protective sac around the spinal cord is sticking out and there is no nerve damage, chances are good that after the child has surgery to close the area, there will be no remaining effects. If the spinal cord is sticking out, the child's legs may be paralyzed. The amount of paralysis depends on where the opening is. The lower the opening is in the back, the less paralysis there is.
Treatment may also include:
- Physical therapy
- Waist or leg braces, walkers, crutches, and other equipment
- Diet and bowel training
- Medicines, tubes, or surgery to help bladder problems
How can I take care of my child?
Follow your child’s healthcare provider's instructions. Ask your provider:
- How and when you will get your child’s test results
- How long it will take for your child to recover, if your child had surgery
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
- What medical specialists your child may need to see
Make sure you know when your child should come back for a checkup.
For more information, contact:
- Spina Bifida Association of America
800-621-3141
https://www.spinabifidaassociation.org/
How can I help prevent spina bifida?
A mother can lower the risk of having a baby with spina bifida by taking folic acid before and during pregnancy. All women of childbearing age should talk with their healthcare provider about a folic acid supplement.
Last modified: 2020-01-06
Last reviewed: 2018-11-26