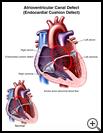
Atrioventricular Canal Defect
________________________________________________________________________
KEY POINTS
- An atrioventricular canal defect is a birth defect of the heart. It causes blood to flow where it should not. The heart has to work harder and it gets bigger.
- This birth defect is usually treated with surgery in childhood.
- Treatment may include medicines and regular follow-up visits.
- Stay up to date with the recommended immunizations (shots) for your child including flu and COVID-19. Ask your healthcare provider about any other vaccines your child or your family may need.
________________________________________________________________________
What is an atrioventricular canal defect?
An atrioventricular canal defect (AVCD) is a birth defect of the heart.
The heart normally has 2 upper chambers (atria) and 2 lower chambers (ventricles). The wall of tissue that separates the right and left sides of the heart is called the septum. A normal heart has 2 heart valves that separate the upper and lower chambers. The valves and septum together are called the atrioventricular canal. Normally the left side of the heart pumps blood to the body, and the right side pumps blood to the lungs.
In AVCD, there are holes in the walls between the chambers of the heart, and the valves that control blood flow may not work well. With AVCD, blood flows where it should not and more blood gets pumped into the lungs. The heart has to work harder and it gets bigger.
AVCD is also called atrioventricular septal defect or endocardial cushion defect.
What is the cause?
The cause of this birth defect is not known. It is most common in babies with Down syndrome.
What are the symptoms?
The symptoms may start at any time from birth to several months after birth. Symptoms may include:
- Not eating well
- Decreased growth
- Trouble breathing
- Heart pounding or irregular heartbeats
- More colds and lung infections
- Gray or bluish color to skin
- Tiring easily
Many defects cause a whooshing sound, called a murmur, as blood moves through the heart. Healthcare providers can hear the murmur with a stethoscope.
How is it diagnosed?
AVCD can be diagnosed before birth, using screening tests to check for birth defects. If the defect is large enough, tests may include:
- An ultrasound, which uses sound waves to show pictures of the baby while it is inside the womb
- An echocardiogram, which uses sound waves (ultrasound) to show pictures of the baby's heart and how well blood is flowing through it after the baby is born
After birth, your child’s healthcare provider will ask about your child's symptoms and medical history and examine your child. In addition to an echocardiogram done after birth, other tests may include:
- A chest X-ray
- An ECG (also called an EKG or electrocardiogram), which measures and records your child’s heartbeat
Sometimes heart catheterization may be needed. A catheter is a very thin tube that is passed through a blood vessel into the heart. The pressure in the chambers of the heart is measured and blood samples can be taken. This helps to tell how big the defect is.
How is it treated?
Your child will need surgery to repair the AVCD. Your baby may need to take medicines until strong enough to have surgery.
If your baby is very sick, or the defect can’t be fixed all at once, your baby may have a procedure to reduce blood flow to the lungs. Your child’s healthcare provider can put a band around the lung artery to make it narrower. Then the heart will not have to work as hard, and the lungs will be protected from high blood pressure. When your child is older, the band can be removed and open-heart surgery done.
How can I take care of my child?
Your child may need to have regular follow-up visits with a specialist in congenital heart disease. In addition:
- Take care of your child’s health. Make sure your child eats a healthy diet and gets enough sleep and physical activity every day. Talk to your older child about the risks of smoking and using e-cigarettes, drinking alcohol, and using drugs.
- Stay up to date with the recommended immunizations (shots) for your child including flu and COVID-19. Ask your healthcare provider about any other vaccines your child or your family may need.
Follow your child’s healthcare provider's instructions. Ask your provider:
- How and when you will get your child’s test results
- How long it will take for your child to recover
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- If your child should take antibiotic medicine to prevent infection before having dental work or procedures that involve the rectum, bladder, or vagina
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
Last modified: 2021-06-25
Last reviewed: 2019-02-25