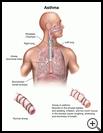
Asthma: Smoking and Your Child
________________________________________________________________________
KEY POINTS
- Asthma is a chronic lung disease that can cause shortness of breath, coughing, wheezing, and sometimes chest tightness.
- Children with asthma who live in a household with people who smoke have more breathing problems, need to take more medicines, and have more emergency room visits than children who live in smoke-free homes.
- Limiting exposure to these triggers can help prevent problems for your child.
________________________________________________________________________
How does tobacco or marijuana smoke affect children with asthma?
Asthma is a long-lasting (chronic) lung disease. It can cause shortness of breath, coughing, wheezing, and sometimes chest tightness.
Asthma symptoms are caused by two different problems in the airways:
- One problem is that the tiny muscles around the airways tighten up, which causes shortness of breath, coughing, wheezing, and sometimes chest tightness.
- The other problem is redness, swelling, irritation, and too much mucus in the airways.
Tobacco and marijuana smoke irritates and damages the airways in several ways. Smoke is made up of chemicals and very small pieces of ash that stay in the air long after the cigarette, pipe, or cigar is out. When a child with asthma breathes in these airborne chemicals and ash, it irritates the lining of the airways. This causes the muscles around the airways to squeeze tight, making it hard for the child to breathe.
Breathing secondhand smoke, also called passive smoking, is also harmful to the lungs. Children who breathe secondhand smoke often have symptoms such as coughing, wheezing and a tight feeling in the chest. Thirdhand smoke is made up of harmful chemicals left on surfaces from tobacco or marijuana smoke. It stays on carpet, floors, walls, clothes, and other surfaces for a long time. Children can be exposed to these chemicals by touching a surface and then touching their mouth or nose.
Even the smell of smoke on clothes can trigger asthma symptoms in a child with sensitive airways. Children with asthma should not spend any time in places where there is smoke. No one should smoke in the home, and no one should smoke in a car that a child with asthma rides in. Airing out cars and homes does not get rid of thirdhand smoke.
Children with asthma who live in a household with people who smoke have more breathing problems, need to take more medicines, and have more emergency room visits than children who live in smoke-free homes. Children who live in a household with people who smoke are also less likely to outgrow their asthma.
E-cigarettes also cause problems. They do not produce water vapor. E-cigarettes produce more, very fine chemical particles than tobacco cigarettes. These chemicals can irritate your child’s lungs and worsen breathing problems, including asthma. The vapor from e-cigarettes may also be harmful to people who are near someone who is vaping, similar to secondhand smoke. For this reason, many cities have passed laws against vaping in public places.
If you or your child smoke or use e-cigarettes, it is important to quit smoking or vaping. Talk to your healthcare provider about ways to quit.
What will help me stop smoking?
The American Lung Association gives the following tips:
- Set a date for quitting.
- Remove cigarettes, ashtrays, matches, and lighters from your home, workplace, and car.
- Keep a supply of low-calorie snacks handy.
- Spend more time in places that don't allow smoking.
- Tell everyone you're going to stop smoking.
- Plan what you'll do instead of smoking.
- Call a friend if you need help.
- Think about using nicotine replacement gum or patches. The nicotine gum or patches help you cut your craving for nicotine. You can also ask your healthcare provider for a prescription medicine to help you quit.
For more information, contact:
- American Lung Association
800-548-8252
https://www.lung.org
Last modified: 2021-07-27
Last reviewed: 2021-06-15