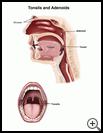
Tonsil and Adenoid Removal in Children and Teens (Tonsillectomy and Adenoidectomy)
________________________________________________________________________
KEY POINTS
- A tonsillectomy and adenoidectomy is surgery to remove the tonsils and adenoids. This procedure may be done to treat breathing or swallowing problems, frequent infections of the tonsils, or other problems.
- Ask your child’s healthcare provider how long it will take to recover and how to take care of your child at home.
- Make sure you know what symptoms or problems you should watch for and what to do if your child has them.
________________________________________________________________________
What is a tonsillectomy and adenoidectomy?
A tonsillectomy and adenoidectomy (T&A) is surgery to remove the tonsils and adenoids in child less than 18 years old.
- Your child has 2 tonsils, one on each side of the back of the throat. They look like reddish, oval-shaped masses and may be easy to see, especially if they are swollen.
- Adenoids are small glands high in the throat behind your child’s nose and the roof of your child’s mouth that cannot be seen without special equipment.
The tonsils and adenoids help the body fight infections such as colds. However, the body's ability to fight infection doesn’t change if they are removed. Removal of the tonsils can help prevent infection of the tonsils. The surgery may also help breathing or swallowing problems.
When is it used?
Reasons for removing just the tonsils or tonsils and adenoids are:
- Obstructive sleep apnea (OSA), usually confirmed with a sleep study in a sleep lab or in your home (polysomnogram), caused by enlarged tonsils that cause breathing problems. Symptoms may include:
- Snoring, trouble breathing, gasping, or choking while your child sleeps
- Pauses in your child’s breathing for at least 10 seconds at a time while sleeping
- Unusual bed wetting
- Daytime sleepiness sometimes seen with older children or teens
- Behavior problems or problems with learning
- Frequent infections of the tonsils that need treatment from your child’s healthcare provider
- At least 3 infections a year for 3 years
- At least 5 infections a year for 2 years
- At least 7 infections in a year
Symptoms may include:
- Fever
- Sore throat
- Mouth sores
- Tender or enlarged lymph nodes in your child’s neck
- An ongoing (chronic) infection of the tonsils that has not improved with treatment after at least 12 weeks. Symptoms may include:
- Enlarged, reddened tonsils
- Sore throat
- Tender or enlarged lymph nodes in your child’s neck
- A build-up of pus (abscess) around one or both tonsils that has not improved with treatment
- Enlarged tonsils (tonsillar hypertrophy) and possibly adenoids that affect speech and swallowing and may cause snoring
Ask your healthcare provider about your choices for treatment and the risks.
How do I prepare my child for this procedure?
- This surgery may be done as an outpatient or inpatient procedure. This means that your child may be able to go home the same day as the surgery, or your child may be in the hospital for one or more days. Talk to your child’s healthcare provider about where your child will have surgery.
- Your child may or may not need to take regular medicines the day of the procedure. Tell your healthcare provider about all medicines and supplements your child takes. Some products may increase the risk of side effects. Ask your healthcare provider if your child needs to avoid taking any medicine or supplements before the procedure.
- Tell your healthcare provider if your child has any food, medicine, or other allergies such as latex.
- Your child’s provider will tell you when your child needs to stop eating and drinking before the procedure. This helps to keep your child from vomiting during the procedure.
- Tell your child’s provider if your child has an infection such as a cold.
- Follow any other instructions your child’s healthcare provider may give you.
- Ask any questions you have before the procedure. You should understand what your child’s healthcare provider is going to do. You have the right to make decisions about your child’s healthcare and to give permission for any tests or procedures.
What happens during the procedure?
Your child will be given a general anesthetic to prevent pain during the procedure. General anesthesia relaxes the muscles and puts your child into a deep sleep.
Your child’s healthcare provider will use a device to keep your child’s mouth open during the procedure. Then your child’s provider will remove the tonsils or tonsils and adenoids from the surrounding tissues. Your child’s provider may use stitches, a burning tool (cautery), a laser, or radio waves to help stop any bleeding.
What happens after the procedure?
The device used to keep your child’s mouth open during the surgery may cause some temporary numbness or soreness in your child’s tongue.
Your child will have a sore throat and be uncomfortable for a few days. It will hurt to swallow, so offer your child soft foods until your child feels better. Limit your child’s activity as advised by your child’s healthcare provider.
As your child’s throat heals and the scabs come off, your child’s throat may bleed. If this happens, have your child spit the blood out. Swallowing the blood may make your child vomit, which can cause more damage to your child’s throat after surgery.
There may be some change in your child’s voice due to the removal of your child’s tonsils and adenoids. This is normal.
Follow your child’s healthcare provider's instructions. Ask your provider:
- How long it will take for your child to recover
- If there are activities your child should avoid and when your child can return to normal activities
- How to take care of your child at home
- What symptoms or problems you should watch for and what to do if your child has them
Make sure you know when your child should come back for a checkup. Keep all appointments for provider visits or tests.
What are the risks of this procedure?
Every procedure or treatment has risks. Some possible risks of this procedure include:
- Your child may have problems with anesthesia.
- Your child may not get enough liquids if your child is unable to swallow.
- Your child may have an infection or bleeding. Your child might need more treatment, possibly surgery, to stop bleeding. Bleeding can happen up to 10 days after surgery.
Ask your healthcare provider how these risks apply to your child. Be sure to discuss any other questions or concerns that you may have.
Last modified: 2022-01-03
Last reviewed: 2020-06-26